Document Processing in Health Care Technology
Health care technology companies process millions of documents every day — prior authorization requests, explanation of benefits, clinical summaries, eligibility verification forms, remittance advice, medical necessity reviews, denial letters, interoperability data packages, the list goes on.
Slow or inaccurate document processing delays patient access decisions, stalls revenue capture, and creates downstream errors that compound across every connected system.
LandingAI transforms documents into highly accurate, verifiable, structured data so teams can reliably automate document-intensive workflows.
Why Agentic Document Extraction for
Health Care Technology
Traceability Across Every Extraction
Every field extracted from a clinical summary, prior auth packet, or remittance document is grounded to its exact location in the source file, giving health IT teams the audit trail required to support compliance reviews and dispute resolution at scale.
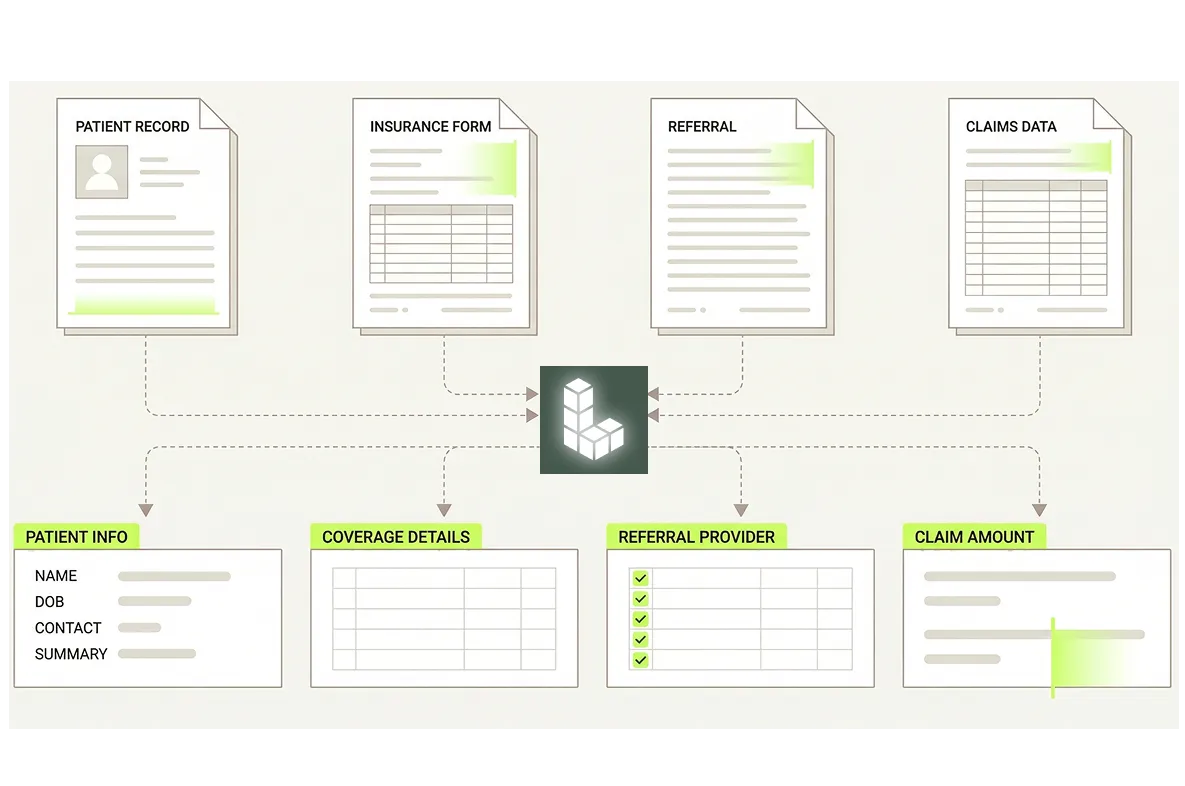
Accuracy Across Inconsistent Document Formats
Health care technology platforms receive documents from hundreds of payer, provider, and clearinghouse sources in inconsistent layouts, scan quality, and structure, and accurate extraction across that variation is what separates a production-grade system from a pilot.
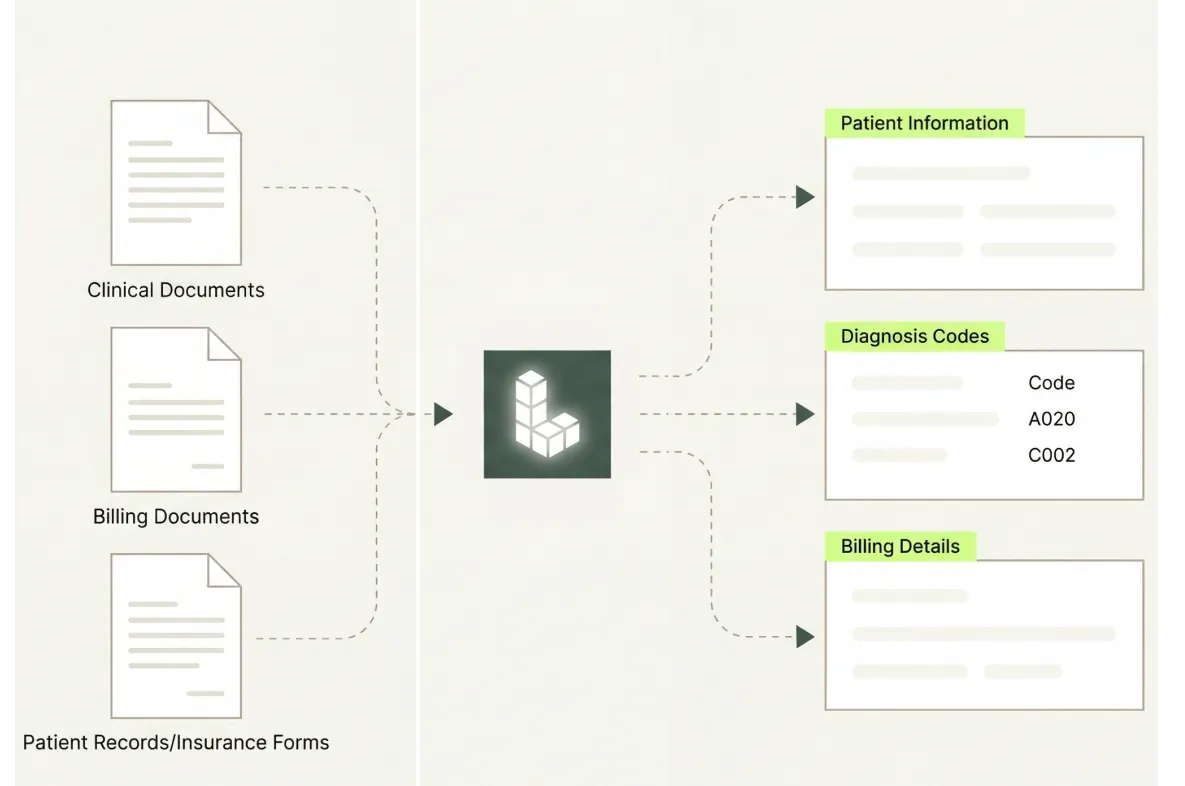
Scale Without Proportional Overhead
Health IT platforms that process authorization requests, claims, or interoperability data at enterprise volume cannot absorb proportional growth in manual review headcount — accurate, automated extraction is the only path to scalable operations.
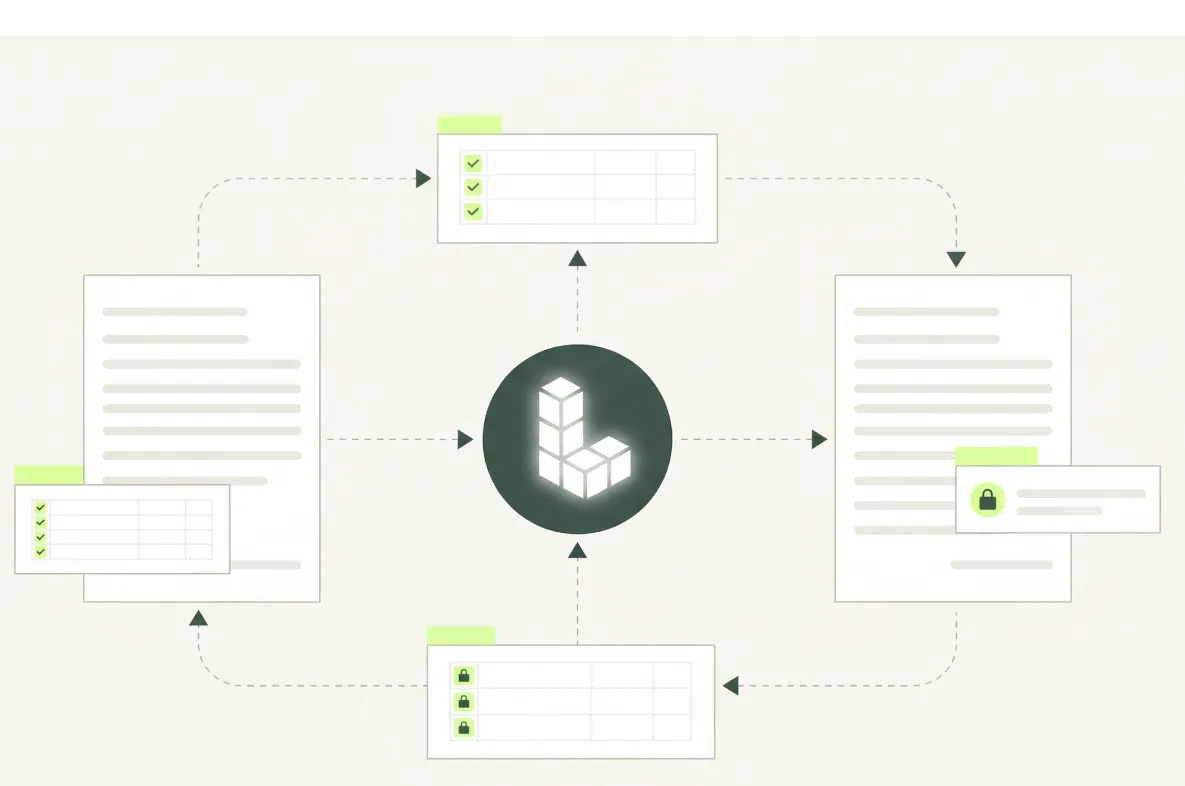
Built for Complex Health Care Technology Documents
Intelligent document processing across EHR and EMR platforms, revenue cycle management, health information exchanges, and telehealth and care coordination technology is extremely difficult due to the sheer diversity of document types, the inconsistent layouts and the domain expertise required. Then add multiple languages, handwriting, photographs, scans and faxes to the complexity.
Accurate parsing of dense tables that span multiple pages and contain merged cells.
Single pipeline for image, slide, document, and spreadsheet file types with 1000+ pages.
Strong recognition of character-based languages, handwriting, checkboxes, stamps and signatures.
Schema-driven field extraction with visual grounding traceable to the original document.
Use cases

Prior Authorization Processing
Extract clinical documentation, medical necessity criteria, diagnosis codes, and supporting records from prior authorization requests, clinical notes, and payer-specific submission forms to accelerate authorization decisions.
Accelerate authorization turnaround, reducing treatment delays that drive member and provider dissatisfaction
Cut manual intake and data entry costs per authorization request
Ensure complete, traceable documentation for every decision to support appeals and compliance audits

Revenue Cycle & Denial Management
Automate extraction of claim data, remittance codes, and denial rationale from explanation of benefits, remittance advice, and denial letters to identify root causes and drive resolution at scale.
Recover revenue faster by identifying and resolving denial root causes across high claim volumes
Reduce labor costs in accounts receivable follow-up and denial rework
Build a complete, structured audit record for every claim cycle to support payer dispute resolution

Clinical Data Onboarding & Interoperability
Ingest and structure patient records, clinical summaries, continuity of care documents, and health information exchange packets to normalize data for downstream EHR, analytics, and care coordination systems.
Accelerate patient data onboarding to reduce time-to-activation for new provider and payer connections
Eliminate manual data reconciliation effort across mismatched clinical document formats
Reduce data quality errors that create downstream coding, billing, and care coordination risk
Trusted for Document-Heavy Health Care Technology Workflows
Agentic Document Extraction enables health care technology companies to automate document-intensive processes that traditionally require manual review.
Agentic Document Extraction has proven to be both accurate and easy to use. We are building on that foundation to deliver reliable, transparent, and scalable automation that our customers can validate and trust.”
View case study →
ADE has significantly outperformed other document extractors we’ve used. It has helped us build an Agentic RAG answer engine, based on unique healthcare institutional content, to offer instant, validated support to medical professionals at the point of care.”
View case study →Our Plan Review Agent has a lot of complicated components under the hood: traversing building code knowledge graphs, reasoning across disciplines and sheets, assessing issues informed by historical projects. None of it works if we can’t trust what came off the page. ADE gave us a reliable foundation, so our team could focus on incorporating our team’s expertise into our compliance reasoning system.”
View case study →
Trust is the product. Accuracy alone isn’t enough at enterprise scale—what matters is provenance, traceability, and control. LandingAI gives us confidence that every extracted value can be traced back to its source, audited, and defended. That’s what makes it deployable in regulated, real-world environments.”
View case study →
Agentic Document Extraction has proven to be both accurate and easy to use. We are building on that foundation to deliver reliable, transparent, and scalable automation that our customers can validate and trust.”
View case study →
ADE has significantly outperformed other document extractors we’ve used. It has helped us build an Agentic RAG answer engine, based on unique healthcare institutional content, to offer instant, validated support to medical professionals at the point of care.”
View case study →Our Plan Review Agent has a lot of complicated components under the hood: traversing building code knowledge graphs, reasoning across disciplines and sheets, assessing issues informed by historical projects. None of it works if we can’t trust what came off the page. ADE gave us a reliable foundation, so our team could focus on incorporating our team’s expertise into our compliance reasoning system.”
View case study →
Trust is the product. Accuracy alone isn’t enough at enterprise scale—what matters is provenance, traceability, and control. LandingAI gives us confidence that every extracted value can be traced back to its source, audited, and defended. That’s what makes it deployable in regulated, real-world environments.”
View case study →

