Document Processing in Life & Health Insurance
Life and health insurers process millions of documents every year — policy applications, attending physician statements, explanation of benefits forms, prior authorization requests, disability claim packets, long-term care assessments, annuity suitability forms, group enrollment files, the list goes on.
Slow document processing delays policy issuance and benefit decisions, eroding customer trust and creating compliance exposure across every line of business.
LandingAI transforms documents into highly accurate, verifiable, structured data so teams can reliably automate document-intensive workflows.
Why Agentic Document Extraction for
Life & Health Insurance
Speed Decisions That Retain Customers
Faster extraction of applicant health data, medical records, and supporting documents compresses underwriting cycle times, reducing the application drop-off that costs carriers significant new business revenue each year.
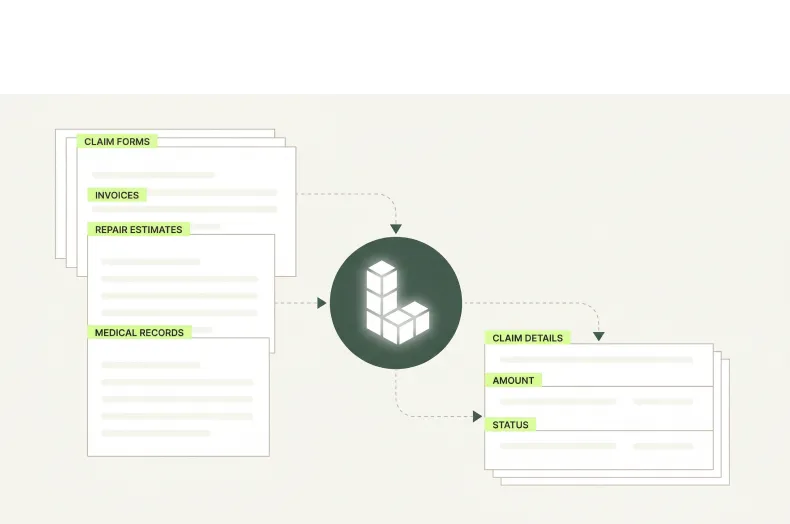
Auditability Built into Every Extraction
Every extracted field is traceable to its exact location in the source document, giving compliance and operations teams a defensible record for suitability reviews, claims adjudication audits, and state regulatory examinations.
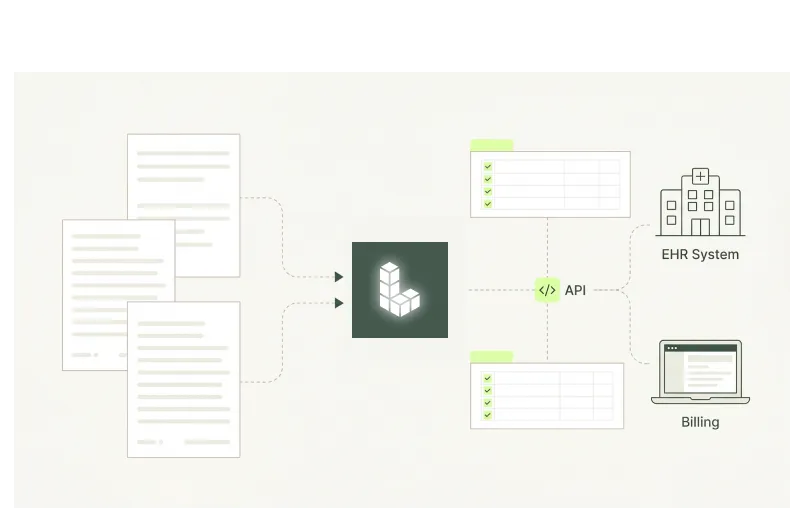
One Pipeline, Every Line
Life, health, disability, annuity, and group benefits operations each generate distinct document types in inconsistent formats — ADE processes all of them through a single pipeline without templates or per-document configuration.
Built for Complex Life & Health Insurance Documents
Intelligent document processing across individual life, group health, disability, and annuity lines is extremely difficult due to the sheer diversity of document types, the inconsistent layouts and the domain expertise required. Then add multiple languages, handwriting, photographs, scans and faxes to the complexity.
Accurate parsing of dense tables that span multiple pages and contain merged cells.
Single pipeline for image, slide, document, and spreadsheet file types with 1000+ pages.
Strong recognition of character-based languages, handwriting, checkboxes, stamps and signatures.
Schema-driven field extraction with visual grounding traceable to the original document.
Use cases

Life Underwriting
Extract applicant health history, risk data, and supporting evidence from applications, attending physician statements, paramedical exam reports, Medical Information Bureau reports, prescription history reports, and motor vehicle records.
Accelerate time-to-offer, reducing in-force application lapse and improving placement rates
Reduce underwriter administrative burden, shifting analyst time to risk judgment rather than data entry
Improve risk selection accuracy with complete, consistently extracted applicant data and a verifiable extraction record

Health Claims Adjudication
Automate extraction of procedure codes, diagnosis codes, provider information, and billed amounts from UB-04 forms, CMS-1500 forms, prior authorization requests, explanation of benefits statements, and clinical notes supporting medical necessity reviews.
Accelerate clean claims throughput, reducing days-in-accounts- receivable and provider abrasion
Cut manual keying costs and rework associated with claim entry errors and resubmissions
Surface billing anomalies and duplicate claims through automated cross-validation of extracted fields

Disability & Long-Term Care Claims
Extract claimant, employer, and attending physician data from short-term and long-term disability claim packets, functional capacity evaluations, treatment plans, and long-term care benefit eligibility assessments to determine benefit entitlement and ongoing case status.
Faster benefit determinations reduce financial hardship for claimants and litigation risk for carriers
Cut per-claim handling costs by automating data capture across multi-part claim packets
Maintain a complete, auditable evidence trail for each benefit decision to support regulatory and legal review
Trusted for Document-Heavy Life & Health Insurance Workflows
Agentic Document Extraction enables life and health insurers to automate document-intensive processes that traditionally require manual review.
Agentic Document Extraction has proven to be both accurate and easy to use. We are building on that foundation to deliver reliable, transparent, and scalable automation that our customers can validate and trust.”
View case study →
ADE has significantly outperformed other document extractors we’ve used. It has helped us build an Agentic RAG answer engine, based on unique healthcare institutional content, to offer instant, validated support to medical professionals at the point of care.”
View case study →Our Plan Review Agent has a lot of complicated components under the hood: traversing building code knowledge graphs, reasoning across disciplines and sheets, assessing issues informed by historical projects. None of it works if we can’t trust what came off the page. ADE gave us a reliable foundation, so our team could focus on incorporating our team’s expertise into our compliance reasoning system.”
View case study →
Trust is the product. Accuracy alone isn’t enough at enterprise scale—what matters is provenance, traceability, and control. LandingAI gives us confidence that every extracted value can be traced back to its source, audited, and defended. That’s what makes it deployable in regulated, real-world environments.”
View case study →
Agentic Document Extraction has proven to be both accurate and easy to use. We are building on that foundation to deliver reliable, transparent, and scalable automation that our customers can validate and trust.”
View case study →
ADE has significantly outperformed other document extractors we’ve used. It has helped us build an Agentic RAG answer engine, based on unique healthcare institutional content, to offer instant, validated support to medical professionals at the point of care.”
View case study →Our Plan Review Agent has a lot of complicated components under the hood: traversing building code knowledge graphs, reasoning across disciplines and sheets, assessing issues informed by historical projects. None of it works if we can’t trust what came off the page. ADE gave us a reliable foundation, so our team could focus on incorporating our team’s expertise into our compliance reasoning system.”
View case study →
Trust is the product. Accuracy alone isn’t enough at enterprise scale—what matters is provenance, traceability, and control. LandingAI gives us confidence that every extracted value can be traced back to its source, audited, and defended. That’s what makes it deployable in regulated, real-world environments.”
View case study →

